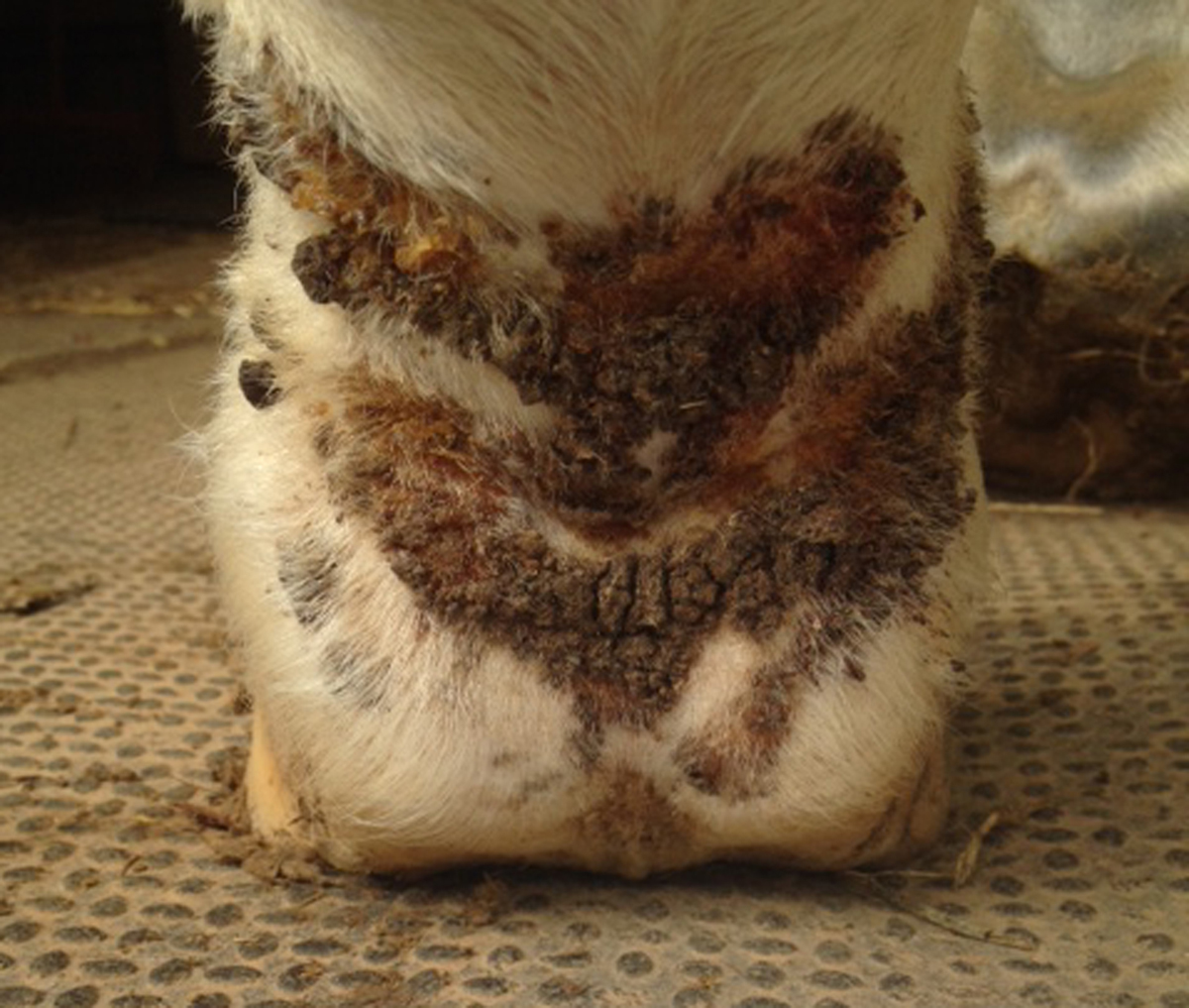
Research author and full professor, Rosanna Marsella, DVM, of the Department of Animal Clinical Sciences at University of Florida (Gainesville) College of Veterinary Medicine, knows Equine Pastern Dermatitis, or greasy heel, is as slippery as its name when it comes to identifying and healing the raw, cutaneous lesions that curse the lower legs of horses, ponies and other equines. The award-winning veterinary dermatologist says, “EPD is not a specific diagnosis. It is a syndrome, caused by a variety of diseases and known by variety of names: scratches, dew poisoning, mud fever, foot rot, cracked heels.”
Equine pastern dermatitis (EPD) is an umbrella term for many kinds of dermatitis or dermatoses affecting that region and was a sore subject at the 2016 eighth World Congress of Veterinary Dermatology, where Dr. Marsella presented her paper, Atopic Dermatitis: What is the Latest in Therapy.
“As we have increased our understanding on the pathogenesis of this complex disease in the last decade, we have become very aware of the importance of skin barrier dysfunction, whether primary or secondary to inflammation. Skin impairment can play an important role in facilitating allergen penetration and increasing the risk for allergic sensitization. More recent therapies have been aimed at restoration of skin barrier impairment,” Dr. Marsella wrote while highlighting that “such a complex disease is best managed with a multi-modal approach which needs to be tailored to each individual case.”
Unlike minor skin conditions that can be brought under control with a simple application of Desitin™ or A&D™ ointment, severe non-responding manifestations of Equine pastern dermatitis (EPD) rob horses and their owners not only of quality of life but of financial health, too.
Such was the case for Phyllis N. of Chesapeake City, MD, and her 24 year-old Thoroughbred gelding, Zo. Phyllis had owned Zo since he was a four year-old and over their two decades together she had struggled with dermatitis and its ensuing scabs to his fetlocks and pasterns.
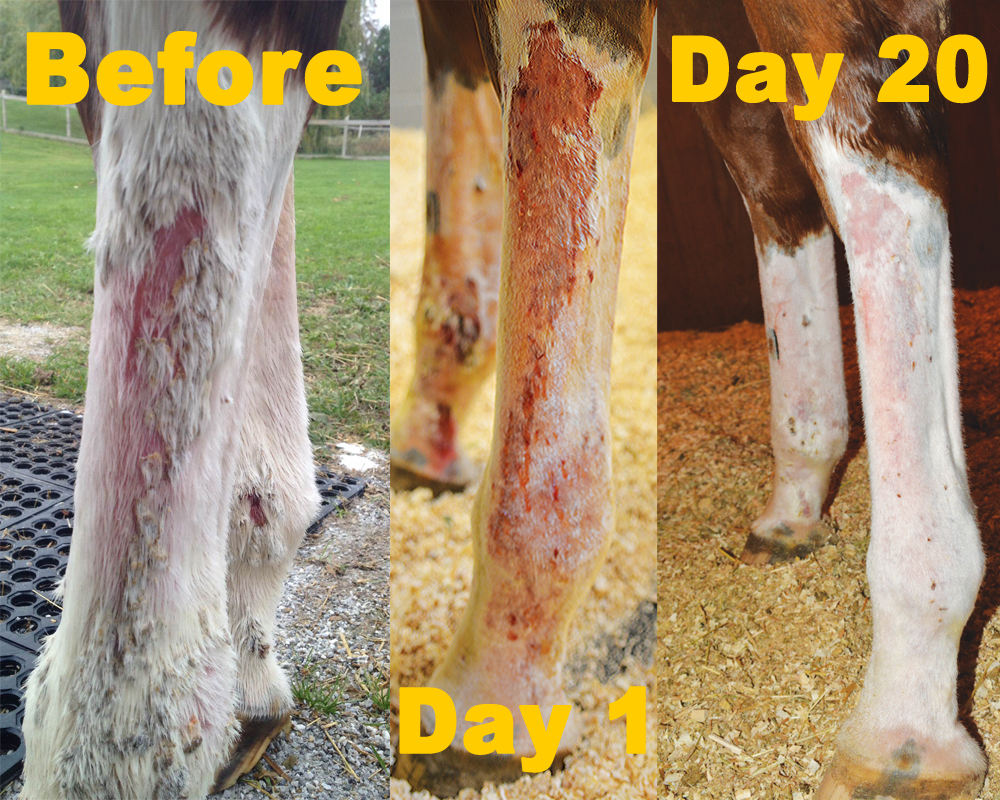
“I scrubbed with Betadine ® (a chemical microbicide) and used vet-prepared ointments that contained steroids and antibiotics. It was becoming a nightmare for my horse and myself,” she said, reaching out to Ray Petterson, president and founder in 2007 of Sox For Horses® pull-on equine leg wear in Tallahassee, FL.
Her story was not unfamiliar. The financial cost of healing EPD, Petterson points out, is compounded by the stress the condition causes and the countless hours of care it demands: “Even more alarming than seeing EPD manifest is — if you’ve faced it in prior seasons – knowing and dreading the long haul ahead seeking out the cause of the problem while your animal continues to suffer.”
Veterinarians conclude that contributing factors to EPD include environmental allergens such as food, insects or pasture growth, as well as the inability of a horse’s immune system to handle pernicious bacteria and fungi. Photosensitivity (the skin’s reaction to UV rays in sunlight) has also been identified as not only a cause but a contributor to worsening cases.
Dr. Marsella said that, while the potential causes are extensive, “First, treat the treatable and address the secondary infections. Once those are resolved then make a reassessment. It is most important to address pastern dermatitis as early as possible. In chronic cases it can be particularly difficult to diagnose the underlying cause.”*
Staphylococcus or ‘staph’ are among the common bacteria driving secondary infection. E. Coli can also be present among other bacteria and fungi. Delaying treatment of sores and wounds sets a dangerous stage for more serious problems, and if a horse’s immune system is compromised, it risks further weakening through the stress of fighting secondary infection. Photosensitivity, allergies to pasture growths, or standing long term in muddy footing contribute to diminishing an immune system’s ability to combat environmental bacteria and fungi, or respond to disease spread animal-to-animal by biting insects.

Equine health experts, like Dr. Erica Lacher of Springhill Equine Veterinary Clinic and Dr. Stephen Soule of Palm Beach Equine Medical, also turn to Sox For Horses for Silver Whinnys and custom bandaging protection. Both agree that environmental contamination can disrupt fragile tissue during healing especially around vulnerable lower limbs and joints.
“You can’t change the weather,” says Petterson, “and you can’t always change where you keep your horse.” But what has changed are the options owners and veterinarians have in leg protection and recovery from painful Equine pastern dermatitis (EPD) lesions.
Here’s why. To propagate, bacteria and fungi require airless environments that trap heat and moisture. “That pretty much sums up the environment offered by the wraps and bandages commonly used to protect legs during healing. Traditional bandaging impedes airflow, holds in moisture and allows heat build-up so you are darned if you wrap and darned if you don’t.”
In a July 2016 interview with Track magazine, Dr. Marsella said she had good results using Silver Whinnys® leg protection: “While not a cure for all cases of EPD, the pull-on equine socks protect the skin and allow second infection to heal. Silver, which has antimicrobial properties and inhibits the growth of bacteria and fungi, is embedded in the yarn used to make this product.”
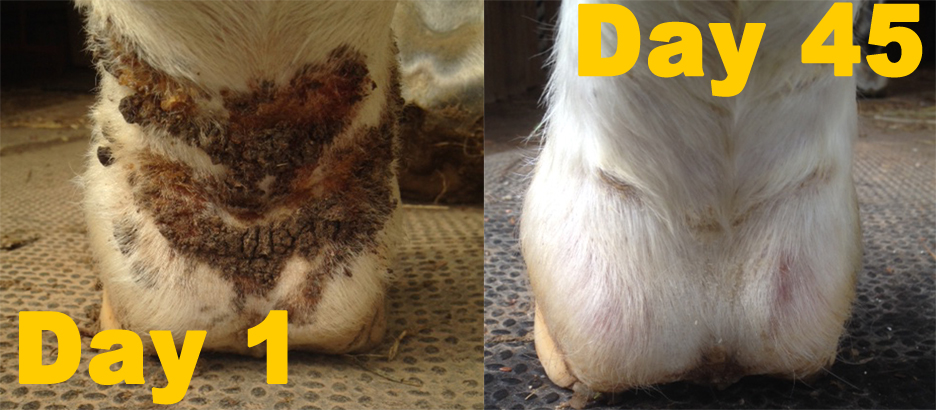
Silver Whinnys allow air to flow across skin surfaces, keeping healing and sensitive tissue dry and cool. Embedded silver in the proprietary yarn used to make these socks is proven to inhibit bacterial and fungal growth while its superior moisture management properties wick moisture away from skin.
“This,” Petterson explains, “accomplishes two vital functions in horse care. Keeping legs cool and skin surfaces dry. Even in mud and wet weather, our horse socks are proven to keep actual skin surface dry and clean.” The double-layered leg wear also protects against direct sunlight and UV rays known to exacerbate and cause EPD.
In comparison, a common ‘barn hack’ of using cotton gym or tube socks for humans he warns, “Is akin to applying a petri dish of infection. You’re not saving money and not operating in the best interest of your horse. Cotton soaks in moisture and provides exactly the breeding ground for infection you need to avoid.”
As for Phyllis and Zo, who turned to Sox For Horses and Silver Whinnys as a last resort?
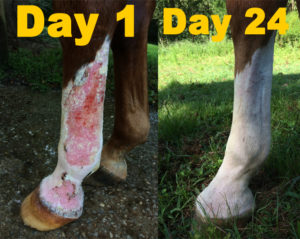
“I started to see improvement at the end of Day One,” she said. “Almost all the scabs are gone now. The few pinpoint-sized ones that remain are very dry. Zo’s hair is returning and the skin on his legs is pink and healthy. He has done very well with his Sox. Some people just will not take the time to check their horses’ legs and put in an effort to help them with their dermatological issues but both Zo and I have gotten better putting them on and off. I change them every 48 hours and know all will be well once he’s fully healed.”
“Greatest product for horses I have ever purchased,” she continued. “I no longer have to fear the onset of late spring and summer when the problem always seemed to recur. Now people ask me what the heck my horse is wearing! I contacted my local vet and shared our story in hopes that he will suggest the socks to other clients. I am a customer for life.”
“Leg protection alone will not cure dermatitis issues,” says the Sox For Horses founder, who was inspired years earlier by the needs of his own horse for leg protection and comfort. “But it will give owners and veterinarians a proven barrier between skin and the environment, and control secondary infections while ruling out other contributing factors.”
The real silver lining is how rapid response and due diligence, combined with leg barrier protection, and the proper medication and researched approach from your veterinarian, can resolve many EPD issues and keep this skin scourge from nipping at your horse’s heels.
* Approach to Equine Pastern Dermatitis, by Rosanna Marsella, DVM, DACVD, published Issue 1, 2014 FAEP The Practitioner, a publication written for the benefit of sharing information among veterinarians and equine health care professionals.

News from the horse industry. Sharing today’s information as it happens. The Northwest Horse Source is not responsible for the content of 3rd party submissions.